Medication-Assisted Treatment in South Florida
Written by Melissa Carmona
& Medically Reviewed by Eric Patterson, LPC
Medically Reviewed
Up to Date
Updated 07/14/2023
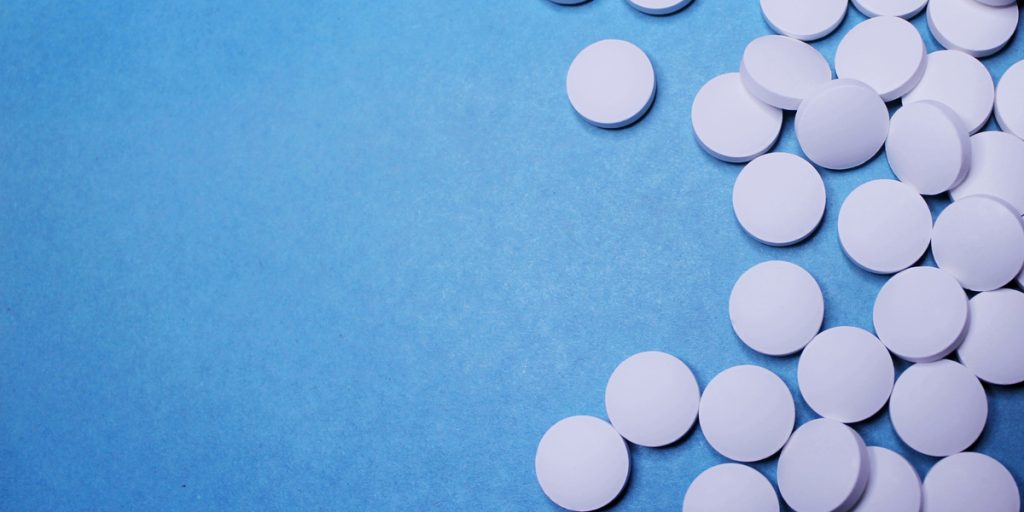
Medication-assisted treatment (MAT) is appropriate for alcohol use disorders and opioid use disorders.
The way that drug and alcohol abuse are treated in South Florida is rapidly changing. For many years, the conventional model of treatment — which promotes strict abstinence while people learn the skills that help keep them sober — was the only one available to people looking for help with substance abuse.
However, over the last two decades, many rehab centers have been able to incorporate helpful medications into treatment drug and alcohol addiction successfully. These medicine-assisted treatment options are now becoming increasingly utilized, and more importantly, increasingly effective at keeping people in treatment longer, preventing overdose deaths and reducing the damaging consequences of drug and alcohol abuse.
What Is Medication-Assisted Treatment?
It’s important to understand the medication-assisted treatment definition. Medication-assisted treatment, or MAT, is the supervised administration of prescribed medications which help reduce physical symptoms of addiction, decrease cravings or prevent withdrawal symptoms.
Most often, MAT is used to aid people who are in treatment for alcohol addiction or opioid addiction.
However, MAT is not meant to take the place of the critically important role of 12-step based programs, psychotherapy and relapse prevention work. As the name suggests, MAT is meant to support the primary psychological treatment and counseling work, rather than replace it. Without counseling support, MAT cannot be fully effective.
Medication-Assisted Treatment for Drug Abuse
The United States Food and Drug Administration (FDA) has approved medications for the treatment of opioid use disorders. These medications can help decrease the intrusive, overwhelming cravings that can affect a person in recovery and redirect their behaviors.
Some of the medications used in MAT are also used to address physical withdrawal symptoms during medical detox. The medications methadone, naltrexone and buprenorphine (including combination buprenorphine and naloxone products like Suboxone) are all approved as medication-assisted treatment for opioid abuse.
Under the guidance of an experienced medical team, taking these medications while attending 12-step groups, therapy sessions, process groups and other treatments can enhance a person’s stability during a vulnerable time as they begin recovery.
Medication-Assisted Treatment for Alcohol Abuse
The FDA has also approved medications to assist in the treatment of alcohol use disorders. The medications disulfiram, acamprosate and naltrexone (including the injectable naltrexone product Vivitrol) are all approved as MAT measures for alcohol use disorders.
Unlike the medication-assisted treatment for opioid abuse, FDA-approved medication-assisted treatment for alcohol use disorders is different than the medications used to treat physical withdrawal symptoms. However, medications used in MAT for both alcohol and opioid use disorders serve the same purpose: to help people in recovery achieve enough stability that their treatment and recovery efforts last longer, are more efficient and are more effective.

Did you know?
Many insurance companies will cover the cost of treatment for drug and alcohol addiction. Verify your insurance benefits with The Recovery Village Palm Beach at Baptist Health.
Medications Used in Medication-Assisted Treatment
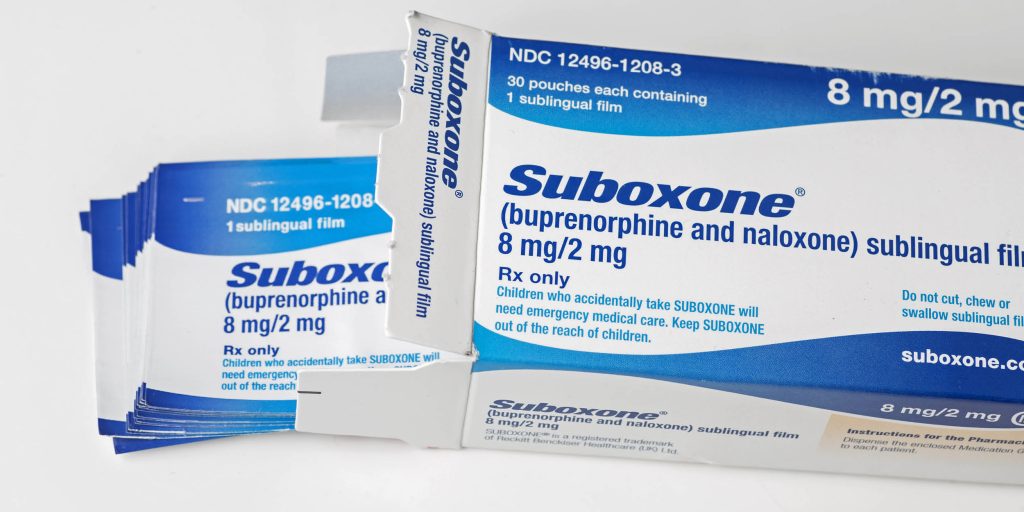
SUBOXONE VS METHADONE
Suboxone and methadone are both treatment options for people suffering from opioid use disorder. There are some key differences between…
VIVITROL VS SUBOXONE
Vivitrol has more convenient dosing than Suboxone, but can only be prescribed with a few important caveats.

METHADOSE
Methadose is a form of methadone that is commonly administered to treat addiction. Learn more about methadose treatment, administration, benefits,…
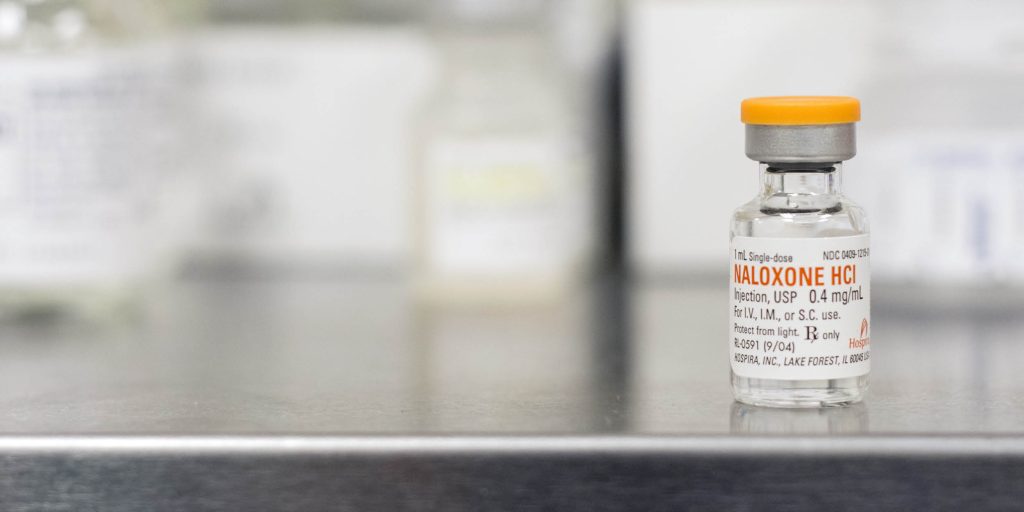
NALOXONE
If an opioid overdose is suspected, naloxone can be administered to save someone’s life. Learn how naloxone reverses opioid overdoses.
BUPRENORPHINE
Buprenorphine is used to relieve withdrawal symptoms and cravings in people in recovery from opioid use. It’s a useful component…
ZUBSOLV
Zubsolv, a drug that contains buprenorphine and naloxone, is used to treat opioid use disorders. It is effective at helping…

METHADONE
Methadone treatment, medication-assistance treatment (MAT) and methadone maintenance treatment (MMT) all use methadone to help with opioid cravings.

DISULFIRAM
Disulfiram is a medication used as an alcohol deterrent. Understanding its use, benefits and risks can help in addressing alcohol…

NALTREXONE
Naltrexone is a medication used in combination with behavioural therapy and social support to alleviate alcohol and opioid dependence.

VIVITROL
A long-acting injectable form of naltrexone, Vivitrol is used in the maintenance treatment of opioid or alcohol dependence

NARCAN
Have you heard of Narcan? If an opioid overdose of a loved one or stranger is suspected, having Narcan nasal…
PROBUPHINE
Probuphine is an implant medication used in the maintenance treatment of opioid dependence. It is part of a complete program…

SUBUTEX
Subutex is a buprenorphine-containing sublingual pill for treating withdrawal from opioid use. Learn how Subutex is used to help people…

CLONIDINE FOR WITHDRAWAL
Clonidine is a common medication for opioid withdrawal treatment, but carries some of its own risks and side effects. Understanding…

SUBOXONE
Suboxone is the most commonly used brand-name formulation of buprenorphine and naloxone. Learn about the role of Suboxone in treating…
SUBLOCADE
Sublocade is an innovative treatment for opioid use disorder. This monthly injection can help to prevent opioid relapse.
BUNAVAIL
Bunavail combines buprenorphine and naloxone. It is an option used for treating withdrawal and cravings in people with opioid use…

ATIVAN FOR ALCOHOL WITHDRAWAL
As one of the gold-standard drugs for alcohol withdrawal treatment, Ativan can help you safely detox and prepare you for…
DOLOPHINE
Dolophine is a FDA-approved medication used in the treatment of severe pain, as well as in the detoxification and maintenance…

ACAMPROSATE
Campral (acamprosate) is a medication used in the maintenance of alcohol abstinence after successful alcohol detoxification.

CASSIPA
As one of the gold-standard drugs for alcohol withdrawal treatment, Ativan can help you safely detox and prepare you for…
ANTIDEPRESSANTS
Antidepressants can be used to treat co-occurring mental health disorders. Learn more about the many different types of antidepressants and…
Success Rates of Medication-Assisted Treatment
Public interest in MAT has grown sharply since the Centers for Disease Control and Prevention and other researchers published data showing that opioid-related overdoses had quadrupled between 1999 and 2010, and that an opioid crisis was emerging.
This renewed public interest coincided with the growing acceptance of vastly underutilized medications to help treat substance use disorders. Studies showed that certain medications could make a meaningful contribution to rehab treatment.
In general, medication-assisted treatment success rates are higher than those of conventional treatment; MAT also appears to decrease the chance of a fatal opioid overdose by at least 50 percent.
Medication-Assisted Treatment Statistics in America
The medication-assisted treatment statistics below highlight important features of substance use disorders. The sheer number of opioid-related overdose deaths demand that the most effective treatment be utilized, and that while the numbers of facilities offering MAT is increasing, the number is still less than 50 percent of all facilities offering substance abuse treatment.
- 70,237 people died from a drug overdose death
- 47,600 people died from an opioid overdose in 2017
- 13,492 substance abuse treatment facilities exist in America as of April 2019
- 5,940 American rehab facilities offer medication-assisted treatment as of April 2019
Medication-Assisted Treatment Program: What to Expect
When entering a MAT program, an initial evaluation is performed by a physician or other medical professional. In this assessment, a series of screening and diagnostic questions can be asked so that a substance use disorder can be identified. This evaluation also identifies co-occurring disorders that may need consideration during treatment. This information will help the clinical team know if the client will be a good candidate for MAT.
It is important to know that medication alone does not treat substance use disorder. Medical experts agree that full treatment of a substance use disorder uses evidence-based psychosocial therapy, education, development of relapse prevention strategies and medication when appropriate.
Once an MAT plan is established (if applicable), how long it continues depends on the individual client, the prescriber and the treatment team. There is no predetermined length of time for MAT, but doses are often decreased after healthy routines are established and emotional sobriety takes root.
If you have been struggling with alcohol or opioid addiction and would like to consider medication-assisted treatment, you have options for rehab. We can help guide you through the process. Call one of our representatives today to get started on your journey to recovery.
We are here when you are ready.
Speak with a Recovery Advocate today to talk about your treatment options.
View Sources
Anton, R et al. “Combined pharmacotherapies and behavioral interventions for alcohol dependence: the COMBINE study: a randomized controlled trial.” JAMA, 2006. Accessed April 24, 2019.
Substance Abuse and Mental Health Administration. “Medication-Assisted Treatment (MAT).” Updated in 2019. Accessed April 25, 2019.
Centers for Disease Control and Prevention. “Opioid Overdose.” Last updated in 2018. Accessed April 25, 2019.
Volkow, N. et al. “Medication-assisted therapies–tackling the opioid-overdose epidemic.” New England Journal of Medicine, 2014. Accessed April 25, 2019.
American Society of Addiction Medicine. “The ASAM National Practice Guidelines Supplement.” Published in 2015. Accessed April 25, 2019.
The AMFAR Foundation for AIDS Research. “Opioid and Health Indicators Database.” (n.d.). Accessed April 25, 2019.
Authorship

 Insurance
Insurance About Us
About Us Our Facility
Our Facility Admissions
Admissions Programs
Programs Medical Detox
Medical Detox Inpatient Rehab
Inpatient Rehab Aftercare & Recovery
Aftercare & Recovery
